Article Text
Abstract
Hospital-associated thromboses (HATs) are a potentially preventable cause of morbidity and mortality. Oxford University Hospitals NHS Foundation Trust was designated a Venous Thromboembolism (VTE) Exemplar Centre by NHS England in 2014. However, following delayed reporting of a potentially preventable HAT in 2015, a benchmarking exercise suggested HATs were being under-reported, and also that the established hospital-wide audits of VTE prevention had significant limitations. The aim of this interventional bundle was to ensure high-quality data for key VTE prevention measures across the hospital, to identify areas for improvement and demonstrate a reduction in the number of potentially preventable HATs over a 2-year period.
The project team engaged with hospital leadership and collaborated with hospital-wide stakeholders. A multifaceted approach was taken and ‘Plan Do Study Act’ cycles were used to test interventions with continuous evaluation of impact. The percentage of inpatients receiving appropriate thromboprophylaxis progressively increased from 94% to 98%. The project did not achieve its secondary aim of a reduction in the number of potentially preventable HATs. Revision of the HAT reporting process resulted in better detection and an initial increase in reporting of potentially preventable HATs, although data suggest that the level of harm from errors is now reducing.
The improvement in overall appropriate thromboprophylaxis is considered to be due to robust audits of appropriate thromboprophylaxis, upskilling of ward pharmacists, improved detection of potentially preventable HATs resulting in additional safety nets such as linking the ‘outcome recommendation’ of the electronic VTE risk assessment directly to electronic prescribing, and increased awareness and education. Combining low-cost actions in a coordinated interventional bundle has produced measurable improvements in our VTE management programme, enhancing patient safety. We believe the model to be sustainable and replicable in other general hospitals.
- quality improvement
- patient safety
- pdsa
- root cause analysis
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.
Statistics from Altmetric.com
Problem
Hospital-associated thrombosis (HAT) is a significant cause of potentially preventable morbidity and mortality. Hospitals in England are required to follow National Institute of Clinical Excellence (NICE) guidance and meet related quality standards in order to reduce the risk of HAT.1 2
Oxford University Hospitals NHS Foundation Trust is one of the largest NHS teaching hospitals in the UK with around 90 000 emergency admissions and 110 000 elective admissions each year. It has 1340 hospital beds, serves a local population of around 800 000 and acts as a regional specialist centre. It has an established venous thromboembolism (VTE) prevention programme and was designated a VTE Exemplar Centre in 2014.
Following significant delay in the identification and reporting of a serious potentially preventable HAT in 2015, a review and benchmarking exercise was undertaken. This indicated that the hospital was reporting fewer potentially preventable HATs than might be expected and that the established hospital-wide audits of VTE prevention measures had significant limitations.
The project’s aim was to identify areas for improvement using high-quality data for key VTE prevention measures, followed by interventions that would result in a reduction in the number of potentially preventable HATs over a 2-year period.
Background
VTE is the collective term for pulmonary embolism and deep vein thrombosis and is associated with significant morbidity and mortality. It has an incidence of 1 in 1000 per annum, and approximately half of VTEs are associated with hospital admissions.3 Thromboprophylaxis has been shown in clinical trials to reduce the risk of VTE by approximately 50% for medical inpatients and up to 70%–80% following orthopaedic surgery.1 4
A national VTE prevention programme was launched in England in 2010 to reduce this hospital-associated morbidity and mortality. The programme is described in detail by Roberts et al.5 The foundation of the programme was national guidance and standards for VTE prevention.1 2 The NICE VTE prevention guidance has been recently updated1 and at the time of this quality improvement project required all adult patients to be VTE risk assessed on admission to hospital using a standardised risk assessment tool. If a patient is assessed to be at increased risk of VTE without significant bleeding risks, the patient is advised to have pharmacological thromboprophylaxis daily while an inpatient. Surgical patients are additionally considered for mechanical thromboprophylaxis. A few selected groups of patients are considered for extended thromboprophylaxis on discharge (total hip and knee replacement, major abdominal cancer surgery). The national VTE prevention programme requires hospitals to record the number of patients who have a VTE risk assessment on admission to hospital (target greater than 95%), and to review all cases of HAT (defined as VTE occurring within 90 days of hospitalisation) to check whether or not the patient received appropriate pharmacological/mechanical thromboprophylaxis daily. If the patient received appropriate thromboprophylaxis daily, then the HAT is reported as not preventable. A potentially preventable HAT reflects that an error occurred (ranging from a single missed dose of pharmacological prophylaxis to multiple missed doses). The level of resultant harm is subsequently graded (mild/moderate/severe). Formal root cause analysis of potentially preventable HATs to identify the causes of the failure allows process changes to reduce the risk of such a failure occurring again.
Evaluating the impact of this national VTE prevention programme is challenging, but there is evidence of a reduction in potentially preventable HATs and mortality associated with VTE.5–7 Reported strategies to improve VTE prevention in hospitals include computer alert systems for VTE risk assessment and prescription, with best results when assessment and prescription are integrated.8–10 An active multifaceted approach has also been advocated,9 and shown to be effective for improving VTE risk assessment rates in medical and surgical admissions.11 12 We therefore planned a multifaceted interventional bundle to optimise hospital-wide patient safety related to VTE prevention.
Measurement
More than 95% of our patients consistently have an electronic VTE risk assessment completed. However, this does not in itself assure that patients actually receive the appropriate thromboprophylaxis daily. Auditing the number of patients who receive appropriate thromboprophylaxis is much more challenging, and it was deemed essential to know this information in order to drive improvement and provide assurance.
Given benchmarking suggested not all potentially preventable HATs were being detected, it was essential to review the HAT reporting process. Individual and aggregate root cause analysis of these incidents would then be a powerful means of identifying weaknesses in the process and allow introduction of additional ‘safety nets’.
The key measurements for assuring and improving patient safety with regard to VTE prevention were considered to be:
Robust audits of appropriate thromboprophylaxis.
The number of potentially preventable HATs and subsequent root cause analysis.
Design
The project team comprised the clinical lead for VTE prevention (Haematology Consultant) and three VTE prevention nurses. Close collaboration with pharmacy and the Electronic Patient Record (EPR) team were seen as essential. Advice and support was sought from the project’s sponsors (Deputy and Associate Medical Directors). Key multidisciplinary stakeholders from various specialties were involved in design and Plan, Do, Study, Act (PDSA) cycles, including quarterly feedback with the hospital’s Thrombosis Working Group, Patient Safety and Clinical Risk Committee and Clinical Effectiveness Committee.
Intervention 1: prioritisation and engagement
A key intervention was to engage the hospital’s leadership to ensure the project was aligned with the hospital’s priorities and to support implementation of hospital-wide changes. Subsequently, the team and deputy medical director engaged with key stakeholders by attending Clinical Governance meetings across the hospital to discuss departmental data (VTE risk assessments, audit and HATs), address concerns and suggest changes to policy.
Intervention 2: robust hospital-wide audits of appropriate thromboprophylaxis
A major limitation of the existing hospital-wide VTE prevention audit was an assumption that thromboprophylaxis was appropriate if patients were prescribed thromboprophylaxis as per the ‘recommended outcome’ of the VTE risk assessment. However, as for many other hospitals nationally, the electronic risk assessment was not directly linked to electronic prescribing and therefore risked being a ‘tick box’ exercise and not being accurately completed. The audit did not cover all clinical areas, occurred only every 6 months and was not independent of the clinical team. The project team therefore planned to develop regular, robust and independent audits of ‘appropriate thromboprophylaxis’.
Intervention 3: improve process for reporting of HATs
As previously described, hospitals in England are required to identify all cases of HAT and analyse whether or not the patient received appropriate thromboprophylaxis. The existing HAT reporting system tasked VTE prevention nurses to search the radiology database weekly for any VTE-positive scans. The nurses checked EPR for prior hospital admissions. The patient’s consultant was then requested to complete a ‘HAT form’. The team reviewed the pathway of HAT reporting with the aim of ensuring all HATs were identified and reported in a timely manner: initial identification of HATs, simplifying process for completion of ‘HAT form’ and methods to ensure timely return.
Intervention 4: continuous specific interventions following root cause analysis of potentially preventable HATs
The VTE prevention team would continue to review root cause analysis and help design and support action plans to try and prevent similar incidents in the future.
Strategy
PDSA cycles were used to trial the interventions. PDSA cycles targeting different aspects of care were run simultaneously. The project team evaluated the impact of the interventions in order to react to any issues and enable further iterations within some of the PDSA cycles.
PDSA 1: audits of ‘appropriate thromboprophylaxis’
The team approached the lead for pharmacy to collaboratively develop robust audits of ‘appropriate thromboprophylaxis’. There were concerns about time pressures for ward pharmacists. Given the potential benefits of robust data and upskilling of ward pharmacists who could then provide an additional daily safety net, pharmacy agreed to pilot one audit.
The lead anticoagulation pharmacist worked closely with the project team to develop training and guidance for ward pharmacists with regard to undertaking a VTE risk assessment. The training materials and audit forms were revised following a pilot. Pharmacists were requested to perform an independent VTE risk assessment and then review the patient’s prescription chart. They were encouraged to seek advice if they were uncertain as to whether a patient had a contraindication to thromboprophylaxis. Any patient considered not to be receiving appropriate thromboprophylaxis was immediately highlighted to the clinical team.
The first audit of ‘appropriate thromboprophylaxis’ was completed July 2016. The audit was conducted in 43 clinical areas, with 10 patients per area. The data were submitted to the VTE prevention team for analysis.
Following positive feedback from ward pharmacists and clinicians, pharmacy agreed to continue to undertake these audits quarterly subject to regular review. Sustainable change was supported by anticoagulants becoming a local hospital Medicines Safety Priority for 2016/2017, and positive feedback and appreciation of the contribution of these audits from the hospital’s Clinical Effectiveness Committee.
The project team explored developing electronic audits of ‘appropriate thromboprophylaxis’ with the informatics team, once the electronic VTE-risk assessment ‘recommended outcome’ was linked directly to electronic prescribing (see PDSA 3). The initial iterations developed over several months suggested that these data would be significantly less robust than independent pharmacy assessment and would also not have the additional benefits of upskilling ward pharmacists. This was therefore not taken further forward.
PDSA 2: root cause analysis of HATs
Following agreement at the hospital’s Clinical Effectiveness Committee, the project team instigated several changes to the HAT detection and reporting process in August 2015:
The informatics team would perform an electronic search of the radiology database daily and email a list of any positive VTE scans to the VTE nurses.
Introduction of electronic prescribing and electronic discharge summaries meant that a significant amount of information was available online without the need to request paper medical records. Completion of the HAT form would remain the responsibility of the patient’s consultant, but the VTE prevention nurses would complete key details of the HAT form from the EPR, simplifying the process for the patient’s admitting consultant and allowing any apparent concerns such as ‘missed doses’ of thromboprophylaxis to be highlighted for particular review.
Clear reporting timeframes and a mechanism to escalate action with support of the Medical Director’s Office. The initial email to the consultant and clinical governance team requested a return deadline of 2 weeks. If the HAT screen was not returned in this time, then a reminder email was sent, with an extended deadline of 1 week. If there was no reply to either of these emails, then a further email was sent copying in the Medical Director’s Office.
Any potentially preventable HATs were to be discussed in the new weekly forum for Serious Incidents Requiring Investigation in order to agree level of harm and appropriate level of investigation.
As will be seen in the Results section, these interventions had significant impact. The process was not significantly changed on review although the VTE Lead delegated more responsibility to VTE prevention nurses for follow-up emails, and the Medical Director’s Office enlisted the help of Clinical Divisional Directors in supporting the return of HAT screens.
PDSA 3: specific interventions following root cause analysis of HATs and feedback from audits
The project team regularly reviewed root cause analysis of potentially preventable HATs in order to look for areas of weakness and additional ‘safety nets’. One of the major subsequent interventions was revision of the electronic VTE risk assessment tool. Root cause analysis of HATs suggested that some might have been prevented if the ‘recommended outcome’ of the electronic VTE risk assessment tool was directly linked to electronic prescribing of thromboprophylaxis. Therefore, the project team met with the hospital’s technology team to link the ‘recommended outcome’ of the electronic risk assessment to an electronic prescribing ‘power plan’. Possible electronic solutions were discussed and developed over a 6-month period. The initial pilot version was revised following feedback from trainee doctors. The first version was implemented December 2016, combined with a hospital ‘safety alert’ and electronic ‘how to’ guide (online supplementary electronic VTE risk assessment details). Continuous review of both initial feedback from doctors and review of subsequent potentially preventable HATs has resulted in further iterations with improved safety nets, for example, an alert is now generated on closure of the patient’s electronic record if the VTE risk assessment is complete but no thromboprophylaxis has been prescribed.
Supplemental material
Other interventions made following root cause analysis of potentially preventable HATs included
Hospital guidelines around peri-procedure pharmacological prophylaxis revised for clarification.
Hospital guideline for thromboprophylaxis and lower limb immobilisation developed.
Introduction of short-term ‘sticker’ in paper medical records to support nursing safety checks for patients wearing mechanical thromboprophylaxis, with subsequent development of an electronic nursing care plan for mechanical thromboprophylaxis.
PDSA 4: increasing training, education and awareness
The hospital’s VTE prevention guidelines were revised in October 2015 and a ‘1 page flowsheet’ was included as an easy practical guide (online supplementary flowsheets). VTE prevention e-learning is mandatory for all clinical staff and the specific e-learning guides for doctors/pharmacists, nurses and midwives were updated. Teaching on mechanical thromboprophylaxis is now integrated in the hospital induction for all nurses and midwifes, as well as the care certificate programme for all clinical support workers.
Supplemental material
VTE prevention awareness was promoted through many platforms: the project team attended the clinical governance meetings of the hospital’s Clinical Divisions at the end of 2015 to discuss local data; members of the project team attended local departmental ‘morbidity and mortality’ meetings; lectures/study sessions for junior doctors, nurses and clinical support workers; use of the hospital’s ‘Safety Alert’ section of the intranet to highlight key messages (online supplementary safety alerts); ward VTE champions and regular newsletters.
Supplemental material
Results
The audits of appropriate thromboprophylaxis undertaken by ward pharmacists provided robust data for this key patient safety measure. They demonstrate an approximate 4% improvement in appropriate thromboprophylaxis over the first year of their introduction which has been sustained over a further 12 months (figure 1). This translates to four additional patients of every 100 admitted receiving appropriate thromboprophylaxis. This improvement is due in part to the actual audits. The audits allowed immediate feedback to the responsible clinical team and resulted in upskilling pharmacists in VTE prevention who then provided an additional daily safety net on the wards. The data are collected per ward, allowing problems specific to a certain area to be highlighted. The other interventions also contributed to the overall improvement in appropriate thromboprophylaxis. Although it is not possible to look at the individual effectiveness of all the interventions, this is discussed further below.
Percentage of inpatients receiving ‘appropriate thromboprophylaxis’ at the hospital. Results from quarterly pharmacy-led audits July 2016 to April 2018, approximately 400 patients included in each audit. ‘Appropriate thromboprophylaxis’ is defined as the patient receiving appropriate pharmacological/mechanical thromboprophylaxis daily, based on hospital guidelines. The improvement in thromboprophylaxis is considered to be a result of the bundle of measures introduced over this period. Of note, linking of the ‘recommended outcome’ of the electronic venous thromboembolism risk assessment directly to electronic prescribing was implemented mid-December 2016 which is associated with the steepest increase in appropriate thromboprophylaxis.
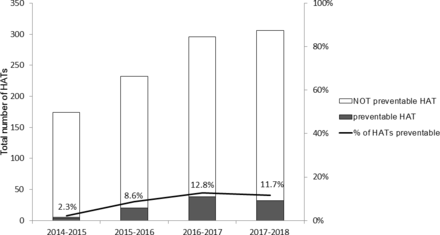
Figure 2 shows the number of HATs reported since April 2014. The main changes in the process for HAT detection and reporting were effected August 2015. Since the introduction of these changes, the number of HATs detected and the percentage of potentially preventable HATs significantly increased (figure 2). Benchmarking suggests that we are now reporting potentially preventable HATs at the level expected.13 The increased detection of potentially preventable HATs resulted in better assurance and ability to identify process weaknesses and implement effective new safety nets. The project team believes that significant errors in care are becoming rarer and this is supported by a reduced number of HATs being reported as a ‘serious incident’ annually (6 in 2015/2016, 8 in 2016/2017 and 0 in 2017/2018).
Annual number of hospital-associated thromboses (HATs) detected at the hospital (based on British financial year April to April, which reflects hospital annual reporting period). It shows the number and percentage of hats which were reported as ‘potentially preventable’, that is, where the patient did not receive daily pharmacological/mechanical thromboprophylaxis that was appropriate based on hospital guidelines. Several changes to the HAT detection and reporting process were instigated in August 2015 resulting in improved detection of HATs overall as well as better recognition of errors of care (potentially preventable HATs).
One of the aims of the new HAT reporting process was to increase the timeliness of reporting, that is, the time taken from requesting the admitting consultant complete the HAT form to its actual completion. We do not have these data recorded prior to August 2015; however, historically there had been a considerable time delay. Interestingly, in the 2.5 years since the introduction of the new HAT process, neither the monthly median reporting time (13.4 days, range 9.9–15.0) nor the monthly average reporting time (15.3 days, range 12.9–19.6) changed significantly. However, there was a decreased requirement to escalate to the Medical Director’s Office for non-returns after the first 16 months (reduction from average of 2.5 HATs a month to 0.75 HATs a month). This reduction has been sustained and suggests increased engagement in the HAT reporting process.
The VTE risk assessment ‘recommended outcome’ was directly linked to electronic prescribing in mid-December 2016. This correlates with the steepest increase in appropriate thromboprophylaxis (figure 1) and suggests that this intervention was significant. To further explore the impact, we performed a retrospective analysis of the VTE risk assessment ‘recommended outcome’ and the actual prescribing of thromboprophylaxis of 138 inpatients (152 admissions). This included 81 admissions in a 4.5-month period before the introduction of the direct link between the risk assessment and electronic prescribing, and 71 admissions in the 4.5 months subsequent. Patients were randomly sampled from those with HATs, as completed HAT forms detailed key information including whether or not thromboprophylaxis had been appropriate. Information was obtained from HAT forms and the EPR. The appropriateness of the prescribed thromboprophylaxis, and the congruence between the ‘recommended outcome’ of the VTE risk assessment and the thromboprophylaxis actually prescribed were reviewed:
Appropriate risk assessment and correct prescription: 55.6% pre, 85.9% post-intervention.
Appropriate risk assessment but prescription incorrect or omitted: 13.6% pre, 5.6% post-intervention.
Inappropriate risk assessment but correct prescription: 9.9% pre, 8.5% post-intervention.
Inappropriate risk assessment and incorrect prescription: 2.5% pre, 0% post-intervention.
Electronic risk assessment not completed: 18.5% pre, 0% post-intervention.
Results of a subgroup analysis of HATS reported as ‘potentially preventable’ (14 pre, 8 post) were
Correct risk assessment and appropriate prescription (but some prophylaxis not administered): 28.6% pre, 87.5% post-intervention.
These results demonstrate that this initiative increased the relevance of the electronic VTE risk assessment and congruence with prescribing. While caution is necessary due to small numbers, subgroup analysis of potentially preventable HATs supports that this initiative should reduce preventable harm from incorrect VTE risk assessment and prescriptions.
Lessons and limitations
Instigating sustainable cross-organisational improvements for VTE prevention and patient safety has required tenacity, resilience and significant time dedication. It would not have been possible without a well-functioning VTE prevention team with supportive close colleagues and hospital leadership. The team’s enthusiasm and momentum was aided by both the positive results and positive feedback including recognition at local Staff Awards.
The collaboration between the VTE prevention team and pharmacy in the hospital-wide audits of appropriate thromboprophylaxis has been very successful. After initial negotiations and agreement to pilot the audit, the positive impact and feedback allowed this collaboration to continue despite time pressure on pharmacy. The value of audits of appropriate thromboprophylaxis has subsequently been recognised by the national VTE prevention programme and a study to examine the feasibility of a standardised National Clinical Audit for VTE prevention is underway (http://www.hqip.org.uk/national-programmes/ncapop-topic-selection/).
The project team was fortunate to work with a highly capable in-house technology team who were able to update the electronic VTE risk assessment, linking the ‘recommended outcome’ to electronic prescribing powerplans and adding subsequent improvements. This has been very successful in increasing the relevance of the risk assessment and supporting appropriate prescribing of thromboprophylaxis.
One of the most challenging aspects of the project was changing the process of HAT reporting. The assertive approach of highlighting concerns such as ‘missed’ doses of thromboprophylaxis, introducing reporting timelines and discussion of all potentially preventable HATs at the hospital’s weekly Serious Incident forum allowed us to pick up significantly more potentially preventable HATs, probably improve the timeliness of reporting compared with previously (anecdotal), and improve decision with regard to grade of harm and level of investigation. However, it was initially met with resistance from some clinicians who questioned the clinical evidence for such oversight especially among competing priorities and limited time. In addition, clinical teams were often anxious about attending the newly established Serious Incident forum. Given this, and the increased number of potentially preventable HATs reported, the haematology lead invested significant unanticipated time in discussing each potentially preventable HAT with the clinical team prior to Serious Incident forum, supporting discussion at this forum and supporting subsequent root cause analysis. This process became less burdensome as the VTE prevention team, hospital consultants and clinical risk practitioners became more familiar with the process of HAT investigation.
Conclusion
At the time of this project, the hospital was already a designated VTE Exemplar Centre. However, a benchmarking exercise undertaken following the delayed reporting of a potentially preventable HAT suggested that HATs were being under-reported. A review of the whole system led to the introduction of a bundle of strategies to improve patient safety.
We took a multi-interventional approach which was supported by previously published work. This led to a 4% sustained increase in ‘appropriate thromboprophylaxis’. This improvement is considered due to feedback of robust data from audits of ‘appropriate thromboprophylaxis’, upskilling pharmacists in VTE prevention, root cause analysis of potentially preventable HATs allowing identification of weakness and leading to additional safety nets, and increased awareness and education of the importance of thromboprophylaxis. This improvement in ‘appropriate thromboprophylaxis’ should ultimately translate to fewer HATs and a reduction in associated morbidity and mortality. The project did not achieve its aim of a reduction in the number of potentially preventable HATs within 2 years. Due to better detection and reporting processes, we actually increased the number of HATs detected and the percentage of potentially preventable HATs in the short term. There is a suggestion that harm resulting from potentially preventable HATs is reducing in severity, that is, the omissions are becoming less serious, although longer follow-up will be required to confirm this.
The project demonstrates the value of continuous monitoring and regular benchmarking of programmes. Review of our ‘exemplar’ VTE prevention programme identified weaknesses which then allowed development of a more effective programme. We believe that the improvements will be sustainable through the mechanisms already put in place. The interventions were low cost as staff were already in place and changes to the electronic VTE risk assessment were done in-house, and such changes could be readily undertaken by other general hospitals. Combining low-cost actions in a coordinated interventional bundle has produced measurable improvements in our VTE prevention programme thereby enhancing patient safety.
Acknowledgments
The authors wish to recognise the significant contribution of the hospital’s pharmacy team (Victoria Price, Mary Collins, Bhulesh Vadher, Paul Devenish, Clare Crowley and ward pharmacists) and Electronic Patient Record technology team (Paul Altman, Scott Harrison, Matthew Wright), support from the hospital’s senior leadership (Clare Dollery, Ivor Byren, Tony Berendt), as well as all the staff at our hospital who aim to ensure daily appropriate thromboprophylaxis for all our patients.
Footnotes
Contributors SS conceived the idea of this Quality Improvement project, analysed data and revised the manuscript. AD collected and analysed data. SK and PC led interventions, collected and analysed data, and wrote the first draft of the manuscript.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Disclaimer The research was supported by the National Institute for Health Research (NIHR) Oxford Biomedical Research Centre (BRC). The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health.
Competing interests None declared.
Patient consent for publication Not required.
Provenance and peer review Not commissioned; externally peer reviewed.