Abstract
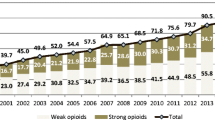
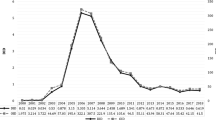
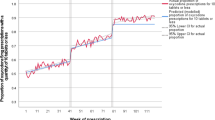
Background Increasing use of opioid analgesics (OA) has been reported worldwide. Objective To compare the use of OA in two countries in order to better understand these trends. Setting Outpatient settings in Australia and The Netherlands. Method We analysed publicly available government data on outpatient OA dispensing over 15 years (2000–2014). We compared dispensing trends for specific OA and explored medical (national clinical guidelines), contextual and policy-related factors to explain differences in use between the two countries. Main outcome measure OA prescribing in Australia and The Netherlands, absolute volume of use, preferred types of opioids and changes over time. Results The average annual increase in OA prescribing was 10% in Australia and 8% in The Netherlands between 2000 and 2014. In 2014, the total use of OA was 10.0 daily defined doses (DDD)/1000 population/day in Australia and 9.4 DDD/1000 population/day in The Netherlands. In Australia, the most commonly prescribed opioids were oxycodone and tramadol, compared to fentanyl and tramadol in The Netherlands. We found differences in prescribing guidelines, culture of prescribing and regulatory frameworks that could explain some of the observed differences. Conclusion OA prescribing has increased remarkably in both countries between 2000 and 2014 but the types of prescribed OA vary. Differences in national evidence-based guidelines influenced the types of OA used. Prescribing culture as well as regulatory policies and costs, may also contribute to the different patterns of OA use.

Similar content being viewed by others
References
Hollingworth SA, Gray PD, Hall WD, Najman JM. Opioid analgesic prescribing in Australia: a focus on gender and age. Pharmacoepidemiol Drug Saf. 2015;24:628–36.
Zin CS, Chen LC, Knaggs RD. Changes in trends and pattern of strong opioid prescribing in primary care. Eur J Pain. 2014;18:1343–51.
Leong M, Murnion B, Haber PS. Examination of opioid prescribing in Australia from 1992 to 2007. Int Med J. 2009;39:676–81.
Ruscitto A, Smith BH, Guthrie B. Changes in opioid and other analgesic use 1995–2010: repeated cross-sectional analysis of dispensed prescribing for a large geographical population in Scotland. Eur J Pain. 2015;19:59–66.
Hamunen K, Paakkari P, Kalso E. Trends in opioid consumption in the Nordic countries 2002–2006. Eur J Pain. 2009;13:954–62.
Henschke N, Kamper SJ, Maher CG. The epidemiology and economic consequences of pain. Mayo Clin Proc. 2015;90:139–47.
Chou R, Turner JA, Devine EB, Hansen RN, Sullivan SD, Blazina I, et al. The effectiveness and risks of long-term opioid therapy for chronic pain: a systematic review for a National Institutes of Health Pathways to Prevention Workshop. Ann Intern Med. 2015;162:276–86.
McCrorie C, Closs SJ, House A, Petty D, Ziegler L, Glidewell L, et al. Understanding long-term opioid prescribing for non-cancer pain in primary care: a qualitative study. BMC Fam Pract. 2015;16:121.
Peppin JF, Cheatle MD, Kirsh KL, McCarberg BH. The complexity model: a novel approach to improve chronic pain care. Pain Med. 2015;16:653–66.
Roxburgh A, Bruno R, Larance B, Burns L. Prescription of opioid analgesics and related harms in Australia. Med J Aust. 2011;195:280–4.
Noble M, Treadwell JR, Tregear SJ, Coates VH, Wiffen PJ, Akafomo C, et al. Long-term opioid management for chronic noncancer pain. Cochrane Database Syst Rev. 2010. doi:10.1002/14651858.CD006605.pub2.
Nicholas R, Roche A, Dobbin M, Lee N. Beyond the paper trail: using technology to reduce escalating harms from opioid prescribing in Australia. Aust N Z J Public Health. 2013;37:139–47.
Australian Statistics on Medicines. Australian Government, Department of Health. https://www.pbs.gov.au/info/browse/statistics#ASM. Accessed 18 April 2017.
GIP databank. Genees- en hulpmiddelen Project [Drug Information Project]. Zorginstituut Nederland, Diemen. http://www.gipdatabank.nl/. Accessed 18 April 2017.
WHO Collaborating Centre for Drug Statistics Methodology. ATC/DDD Index 2015. www.whocc.no/atcddd. Accessed 18 April 2017.
Medicare Australia. Pharmaceutical benefits schedule item reports. http://medicarestatistics.humanservices.gov.au/statistics/pbs_item.jsp. Accessed 18 April 2017.
GIP databank. Genees- en hulpmiddelen Informatie Project [Drug Information Project]. Aantal DDD's per gebruiker 2000–2014 voor ATC-subgroep N02A: Opioiden [DDDs per user 2000–2014 for ATC subgroup N02A: Opioids]. Zorginstituut Nederland, Diemen. www.gipdatabank.nl/database.asp. Accessed 18 April 2017.
Moulds R, Briscoe P, Foreman L, Halliwell R, Hopper I, Johnstone J, et al. Therapeutic guidelines: analgesic. 2012, Version 6. Therapeutic Guidelines Limited. www.tg.org.au. Accessed 18 April 2017.
de Jong L, Janssen PGH, Keizer D, Köke AJA, Schiere S, van Bommel M, et al. NHG-Standaard Pijn: Nederlands Huisartsen Genootschap 2015 [NHG Guideline Pain: Dutch College of General Practitioners 2015]. https://www.nhg.org/standaarden/volledig/nhg-standaard-pijn. Accessed 18 April 2017.
Verduijn MM, Folmer H. Farmacotherapeutische Richtlijn Pijnbestrijding [Pharmacotherapeutic Guideline Analgesic]. Nederlands Huisartsen Genootschap 2007. https://www.henw.org/archief/volledig/id918-ftr-pijnbestrijding.html. Accessed 18 April 2017.
Garbe E, Jobski K, Schmid U. Utilisation of transdermal fentanyl in Germany from 2004 to 2006. Pharmacoepidemiol Drug Saf. 2012;21:191–8.
Kenan K, Mack K, Paulozzi L. Trends in prescriptions for oxycodone and other commonly used opioids in the United States, 2000–2010. Open Med. 2012;6(2):e41–7.
Harrison CM, Charles J, Henderson J, Britt H. Opioid prescribing in Australian general practice. Med J Aust. 2012;196:380–1.
Hollingworth SA, Symons M, Khatun M, Loveday B, Ballantyne S, Hall WD, et al. Prescribing databases can be used to monitor trends in opioid analgesic prescribing in Australia. Aust N Z J Public Health. 2013;37:132–8.
Svendsen K, Borchgrevink P, Fredheim O, Hamunen K, Mellbye A, Dale O. Choosing the unit of measurement counts: the use of oral morphine equivalents in studies of opioid consumption is a useful addition to defined daily doses. Palliat Med. 2011;25:725–32.
Nielsen S, Degenhardt L, Hoban B, Gisev N. Comparing opioids: a guide to estimating oral morphine equivalents (OME) in research. NDARC Technical Report No. 329. Sydney: National Drug and Alcohol Research Centre; 2014.
Roxburgh A, Hall WD, Burns L, Pilgrim J, Saar E, Nielsen S, Degenhardt L. Trends and characteristics of accidental and intentional codeine overdose deaths in Australia. Med J Aust. 2015;203:2991–7.
De Maeseneer JM, van Driel ML, Green LA, van Weel C. The need for research in primary care. Lancet. 2003;362(9392):1314–9.
Holliday S, Magin P, Dunbabin J, Oldmeadow C, Lintzeris N, Attia J, et al. An evaluation of the prescription of opioids for chronic nonmalignant pain by Australian General Practitioners. Pain Med. 2013;14:62–74.
Mossialos E, Wenzl M, Osborn R, Anderson C. International Profiles of Health Care Systems, 2014: Australia, Canada, Denmark, England, France, Germany, Italy, Japan, The Netherlands, New Zealand, Norway, Singapore, Sweden, Switzerland, and the United States. The Commonwealth Fund, January 2015. http://www.commonwealthfund.org/publications/fund-reports/2015/jan/international-profiles-2014. Accessed 18 April 2017.
van Ginneken E. Perennial health care reform—the long Dutch quest for cost control and quality improvement. N Engl J Med. 2015;373:885–9.
Gauld N, Bryant L, Emmerton L, Kelly F, Kurosawa N, Buetow S. Why does increasing public access to medicines differ between countries? Qualitative comparison of nine countries. J Health Serv Res Policy. 2015;20:231–9.
Seamark D, Seamark C, Greaves C, Blake S. GPs prescribing of strong opioid drugs for patients with chronic non-cancer pain: a qualitative study. Br J Gen Pract. 2013;63(617):821–8.
Hutchinson K, Moreland AM, de Williams AC, Weinman J, Horne R. Exploring beliefs and practice of opioid prescribing for persistent non-cancer pain by general practitioners. Eur J Pain. 2007;11:93–8.
McKinlay JB, Trachtenberg F, Marceau LD, Katz JN, Fischer MA. Effects of patient medication requests on physician prescribing behavior: results of a factorial experiment. Med Care. 2014;52:294–9.
Green DJ, Bedson J, Blagojevic-Burwell M, Jordan KP, van der Windt D. Factors associated with primary care prescription of opioids for joint pain. Eur J Pain. 2013;17:234–44.
Campbell G, Nielsen S, Larance B, Bruno R, Mattick R, Hall W, et al. Pharmaceutical opioid use and dependence among people living with chronic pain: associations observed within the pain and opioids in treatment (POINT) cohort. Pain Med. 2015;16:1745–58.
Burgess DJ, Crowley-Matoka M, Phelan S, Dovidio JF, Kerns R, Roth C, et al. Patient race and physicians’ decisions to prescribe opioids for chronic low back pain. Soc Sci Med. 2008;67:1852–60.
Anderson KO, Green CR, Payne R. Racial and ethnic disparities in pain: causes and consequences of unequal care. J Pain. 2009;10:1187–204.
Holliday S, Morgan S, Tapley A, Dunlop A, Henderson K, van Driel M, et al. The pattern of opioid management by Australian general practice trainees. Pain Med. 2015;16:1720–31.
Broekmans S, Dobbels F, Milisen K, Morlion B, Vanderschueren S. Medication adherence in patients with chronic non-malignant pain: is there a problem? Eur J Pain. 2009;13:115–23.
Rosser BA, McCracken LM, Velleman SC, Boichat C, Eccleston C. Concerns about medication and medication adherence in patients with chronic pain recruited from general practice. Pain. 2011;152:1201–5.
McCracken LM, Hoskins J, Eccleston C. Concerns about medication and medication use in chronic pain. J Pain. 2006;7:726–34.
Hall J. Australian Health Care—the challenge of reform in a fragmented system. N Engl J Med. 2015;373:493–7.
Breekveldt-Postma NS, Penning-van Beest FJ, Herings RM. Utilisation pattern of fentanyl transdermal system in The Netherlands. Pharmacoepidemiol Drug Saf. 2005;14:129–34.
Medicijnkosten [Costs of medicines]. Zorginstituut Nederland, Diemen. http://www.medicijnkosten.nl/. Accessed 18 April 2017.
Pharmaceutical Benefits Scheme. Australian Government Department of Health. http://www.pbs.gov.au/browse/body-system?depth=2&codes=n02 Accessed 18 April 2017.
Jammal W, Gown G. Opioid prescribing pitfalls: medicolegal and regulatory issues. Aust Prescr. 2015;38:198–203.
Hobbs T, Baggoley C, Aloizos J, Anns M, Ballantyne S, Bevan V, et al. Opioids roundtable outcomes statement. Canberra: Australian Government Department of Health; 2015.
KNMG. Richtlijn Elektronisch voorschrijven [Guideline Electronic Prescribing]. Utrecht: Koninklijke Nederlandsche Maatschappij tot bevordering der Geneeskunst; 2013.
Acknowledgements
We thank the Australian Government Department of Health and the Dutch National Health Care Institute for providing freely accessible data on medicine dispensing.
Funding
Francisca Wagemaakers was granted a UMC Utrecht Internationalization Committee Grant for strategic network development.
Conflicts of interest
All authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wagemaakers, F.N., Hollingworth, S.A., Kreijkamp-Kaspers, S. et al. Opioid analgesic use in Australia and The Netherlands: a cross-country comparison. Int J Clin Pharm 39, 874–880 (2017). https://doi.org/10.1007/s11096-017-0492-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-017-0492-9